AIDS is a life-threatening disease affecting 38 million people worldwide. Currently, antiretroviral therapy (ART) is the only therapeutic way to suppress HIV in blood. But, HIV still persists in the blood in the dormant form and latently infects the CD+4 T cells. As it cannot be recognized by the immune system, there is no therapeutic way to eliminate them. ART is not the permanent cure for AIDS as the reservoir of latent HIV always persists in the body, creating an obstacle in treatment/therapy.
Scientists and researchers from the University of Now, scientists from the University of North Carolina at Chapel Hill and Emory University used a compound known as AZD5582 to activate the CD+4 T cells in the body with no toxicity. The work published in Journal Nature provides experimental, investigational findings in animal models.

“Previously, no one had successfully tested a latency reversal molecule in humans or in an animal model with human cells demonstrating systemic HIV induction in peripheral blood, in resting CD4+ T cells from multiple tissues, and then replicated this success in a completely different species infected with a different virus,” said co-senior author J. Victor Garcia, Ph.D., director of the International Center for the Advancement of Translational Science, professor of medicine and microbiology & immunology at the UNC School of Medicine.
Researchers suggested the theory of “Shock and kill,” which provides an increased expression of viral genes (shock) and killed by other immune cells (kill) after being recognized by the immune system. The first study by Nixon et al. focused on novel drug molecule, IAP inhibitor called AZD5582, which activates a latent reservoir of viral cells by triggering the transcription factor NF-κB- an instigator of HIV gene expression. The experimental study was conducted on “Humanized” animal models taken (mice and monkeys). Both animal groups were already receiving an “Antiretroviral therapy.”
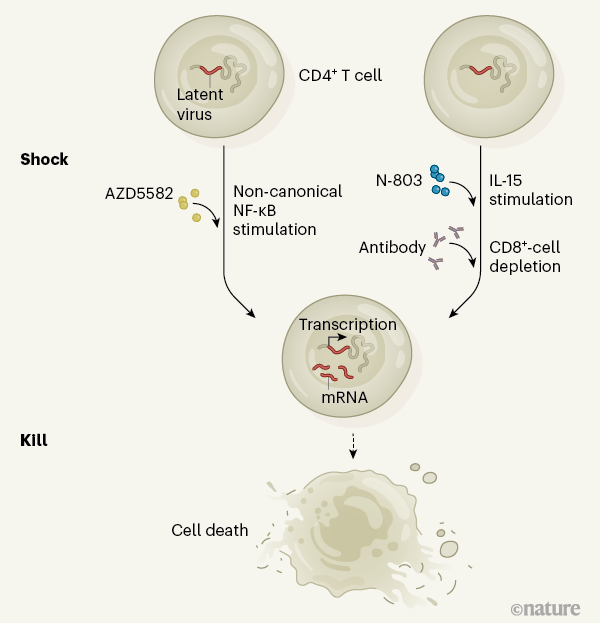
In the second study, McBrien et al. utilizes the combination of depletion of CD+8 T cells by antibiotic mediation and then con-currently administered a drug called N-803 to activate strongly, an IL-15 (Interleukin-15), which triggers HIV gene expression. This combined immunogenic intervention provided the synergistic effect and proved to be the best strategy for HIV therapy.
The Patent application No. WO2019246520A1, filed by the University of North Carolina at Chapel Hill, discloses novel methods to cure HIV. In particular, amino bisphosphonates are disclosed as latency-reversing agents (LRAs), and methods to cure HIV by administering to a subject a combination of bisphosphonates and γδ T cells are provided. In some embodiments, these interventions may be combined with other latency-reversing agents, e.g., histone deacetylase (HD AC) inhibitors, and other immunotherapeutics for HIV clearance (e.g., broadly HIV -neutralizing antibodies).

