
3D Printed Living Skin is now a reality
- Jan 31, 2020
- 0 Comments
Technology advancements nowadays are more welcome in the field of medicines. Biology is far more complicated than simple systems made in the lab. Researchers have recreated biology in tissue engineering with the development of techniques like 3-D printing and 3-D bioprinting. Now grafts are more natural, like our skin produced by the body.
Commercially available grafts mostly slough off and do not have vasculature, i.e., blood vessels required for communications between host and grafts. However, since blood vessels feed the graft from the host with blood and remove other harmful metabolites from blood, that’s the challenge Researchers, and Engineers have overcome recently.
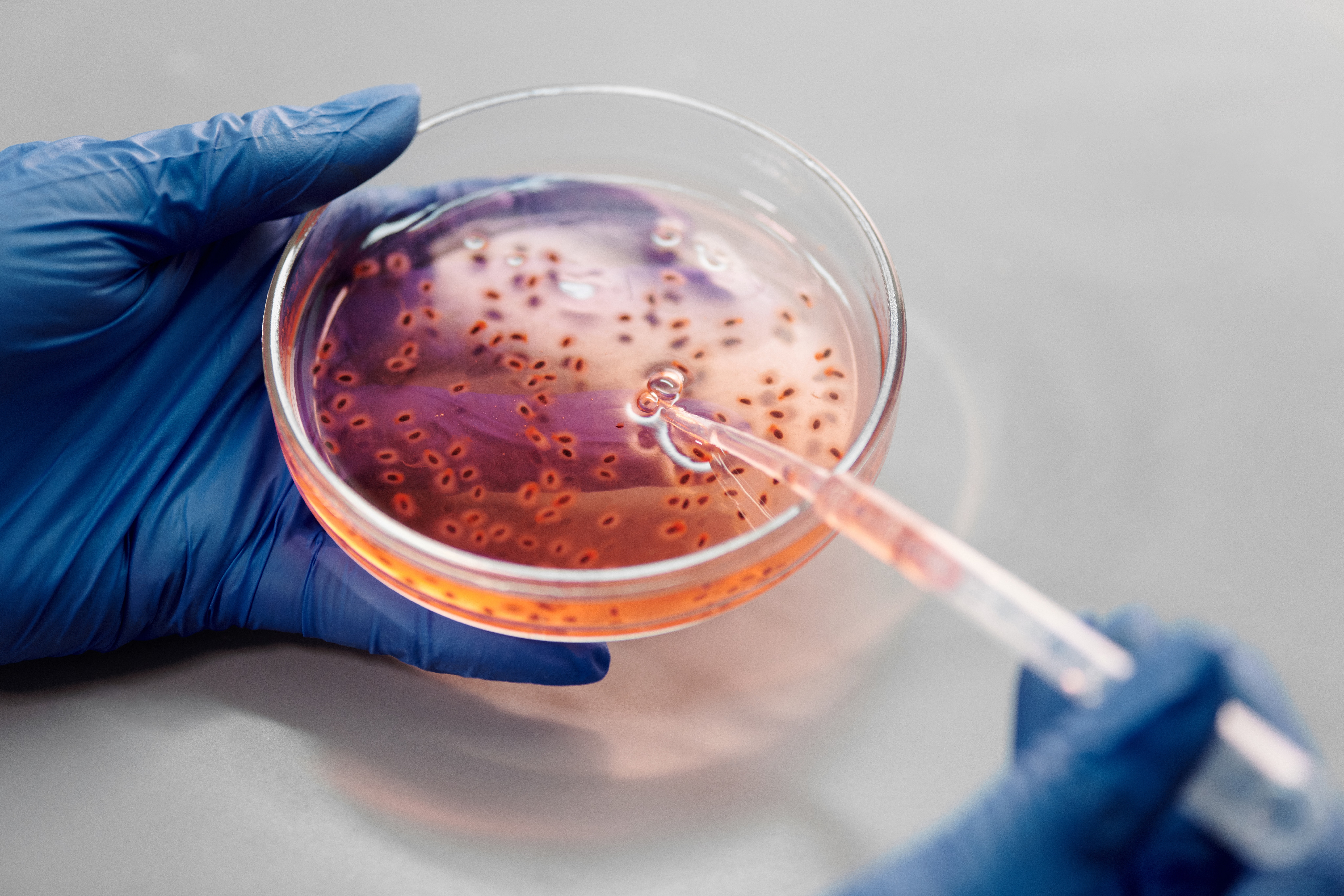
An Indian-origin professor and his team successfully created the living skin tissue with vasculature printed in it at Rensselaer Polytechnic Institute, New York, USA. They developed a skin-like graft tissue by combining human endothelial cells, melanocytes, and human pericyte cells, including other ingredients like animal collagen and other structural cells. In collaboration with Yale University, Researchers incorporated it into a mouse (host). They got desired results as the incorporated skin cells formed vasculature and integrated into the host nicely within a few weeks. The vessels in the skin printed by Researchers connected and communicated well with the mouse’s own blood vessels.
3-D printed skin is an advancement with the hope of preventing blood-rejected grafts since blood vessels are a crucial factor in supplying blood and nutrients from a host to the graft to keep it “alive.” Professor Pankaj Karande explained: "Right now, whatever is available as a clinical product is more like a fancy Band-Aid. It provides some accelerated wound healing, but eventually, it just falls off; it never really integrates with the host cells."
These skin print grafts will address the problems of people suffering from skin burns, wounds induced by diabetes, or ulcers and accelerate the healing process. The work has been published in the journal Tissue Engineering Part A.

The next step in this significant development would be to create modified donor skin cells using gene-editing CRISPR technology to match the recipient’s body, thereby reducing the chances of graft rejection.
The Patent application US20170072111A1, titled “Skin printing and auto-grafting,” assigned to Dermagenesis LLC, discloses the processing of all harvested skin cells taken from a healthy donor site on the patient with the wound to construct a customized skin graft product to be auto-grafted onto the wound. Production of a customized skin graft preferably is accomplished by operation of a three-dimensional (“3D”) printer, which is supplied with substrate material and autologous skin cells. It “prints” the supplied skin cells onto an agar plate or some other surface, wherein a quantity of living donor skin cells harvested from a non-wound area of a patient includes human fibroblasts, keratinocytes, ECM proteins, growth factors, cytokines, and collagen or another scaffold-building material.
Non-patent literature, titled “Three Dimensional Bioprinting of a Vascularized and Perfusable Skin Graft Using Human Keratinocytes, Fibroblasts, Pericytes, and Endothelial Cells,” published in the “Journal Tissue Engineering Part A” on December 3, 2019, discloses multilayered skin substitutes comprising human endothelial cells, pericyte cells, animal collagen, and structural cells, collectively known as (bio-inks) for the treatment of nonhealing cutaneous ulcers. In this study, it was described the fabrication of an implantable multilayered vascularized bioengineered skin graft using 3D bioprinting.

